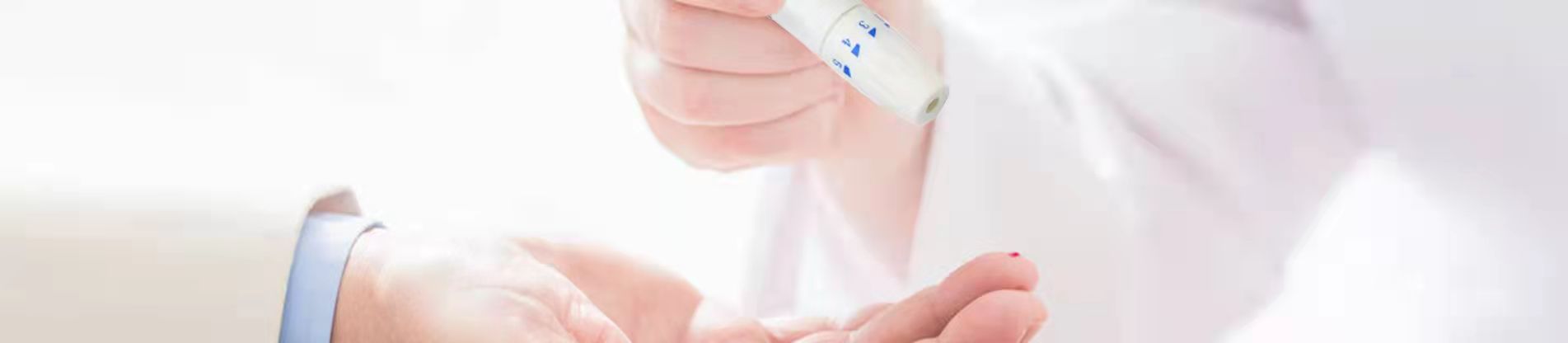
Regular blood glucose monitoring is the most important thing you can do to manage type 1 or type 2 diabetes. You’ll be able to see what makes your numbers go up or down, such as eating different foods, taking your medicine, or being physically active. With this information, you can work with your health care team to make decisions about your best diabetes care plan. These decisions can help delay or prevent diabetes complications such as heart attack, stroke, kidney disease, blindness, and amputation. Your doctor will tell you when and how often to check your blood sugar levels.
Most blood sugar meters allow you to save your results and you can use an app on your cell phone to track your levels. If you don’t have a smart phone, keep a written daily record like the one in the photo. You should bring your meter, phone, or paper record with you each time you visit your health care provider.
How to Use a Blood Sugar Meter
There are different kinds of meters, but most of them work the same way. Ask your health care team to show you the benefits of each. In addition to you, have someone else learn how to use your meter in case you’re sick and can’t check your blood sugar yourself.
Below are tips for how to use a blood sugar meter.
Make sure the meter is clean and ready to use.
After removing a test strip, immediately close the test strip container tightly. Test strips can be damaged if they are exposed to moisture.
Wash your hands with soap and warm water. Dry well. Massage your hand to get blood into your finger. Don’t use alcohol because it dries the skin too much.
Use a lancet to prick your finger. Squeezing from the base of the finger, gently place a small amount of blood onto the test strip. Place the strip in the meter.
After a few seconds, the reading will appear. Track and record your results. Add notes about anything that might have made the reading out of your target range, such as food, activity, etc.
Properly dispose the lancet and strip in a trash container.
Do not share blood sugar monitoring equipment, such as lancets, with anyone, even other family members. For more safety information, please see Infection Prevention during Blood Glucose Monitoring and Insulin Administration.
Store test strips in the container provided. Do not expose them to moisture, extreme heat, or cold temperatures.
Recommended Target Ranges
The following standard recommendations are from the American Diabetes Association (ADA) for people who have diagnosed diabetes and are not pregnant. Work with your doctor to identify your personal blood sugar goals based on your age, health, diabetes treatment, and whether you have type 1 or type 2 diabetes.
Your range may be different if you have other health conditions or if your blood sugar is often low or high. Always follow your doctor’s recommendations.
Below is a sample record to discuss with your doctor.
Two cells below ADA targets for Blood sugar labels Before meals 80 to 130 mg/dl and 1 to 2 hours after meals below 180 mg/dl. 
Getting an A1C Test
Make sure to get an test at least twice a year. Some people may need to have the test more often, so follow your doctor’s advice.
A1C results tell you your average blood sugar level over 3 months. A1C results may be different in people with hemoglobin problemsexternal icon such as sickle cell anemia. Work with your doctor to decide the best A1C goal for you. Follow your doctor’s advice and recommendations.
Your A1C result will be reported in two ways:
A1C as a percentage.
Estimated average glucose (eAG), in the same kind of numbers as your day-to-day blood sugar readings.
If after taking this test your results are too high or too low, your diabetes care plan may need to be adjusted. Below are ADA’s standard target ranges:
Sample table with three headers labeled ADA’s target, my goal, and my results. ADA’s Target column has two cells labels A1C is below 7% and eAG is below 154 mg/dl. The remaining cells under My Goal and My Results are empty.
Questions To Ask Your Doctor
When visiting your doctor, you might keep these questions in mind to ask during your appointment.
What is my target blood sugar range?
How often should I check my blood glucose?
What do these numbers mean?
Are there patterns that show I need to change my diabetes treatment?
What changes need to be made to my diabetes care plan?
If you have other questions about your numbers or your ability to manage your diabetes, make sure to work closely with your doctor or health care team.
Reference
CDC Centers for Disease Control and Prevention
Post time: Jun-27-2022